|
Sign and symptom of Rheumatoid Arthritis:What are they trying to tell you?The major hallmark sign and symptom of Rheumatoid arthritis is the presence of one or more tender, swollen, stiff joints for at least 6 weeks. The swelling and tenderness begins without a known injury. Joints:Another sign and symptom of rheumatoid arthritis is that the stiffness lasts longer than 30 min., often an hour or more in the morning or after inactivity.
Rheumatoid arthritis (RA) generally occurs in a symmetrical manner, which means that if one knee or hand is involved, the other hand or knee is too.
RA often affects the finger joints closest to the palm and the wrist joints. Other common sites of RA include the ball of the foot, toes, knees, hips, neck, shoulders, elbows and ankles are sometimes affected. In contrast, arthritis in the fingertips is usually due to osteoarthritis.
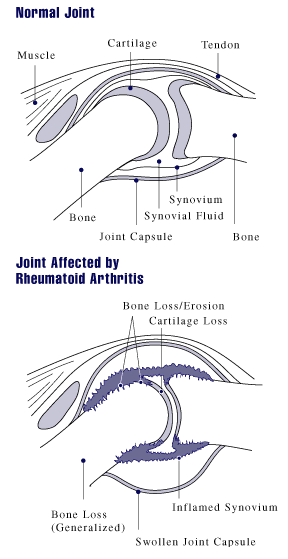
A sign and symptom of rheumatoid arthritis is that inflammation of a particular joint in rheumatoid arthritis patients usually lasts for at least several weeks to months or years. In contrast, joint pain due to lyme disease migrates from joint to joint daily, within a few days or weekly. This diagram of a healthy joint and a joint of a rheumatoid arthritis patient shows the difference in joint space and size of joint membrane. The swollen joint of the RA patient is often spongy to the touch, warm (compared to surrounding area) and tender or painful with pressure. As RA progresses, the pannus or swollen membrane often eats away the cartilage at the end of the bone and may cause deformities.
Joint Damage: As the disease progresses, there can be changes on the surfaces of the joints that can be detected by X-rays. Blood tests:There are several blood tests that help a doctor decide whether you’re likely to have rheumatoid arthritis (RA). The first set checks to see if you make certain specific antibodies because they’re often found in RA patients at high levels. The second set measures the amount of inflammation. Rheumatoid Factor: Rheumatoid factor measures how many of one type of your antibodies (IgM, sometimes IgA) binds to a second type of your antibodies (IgG). Initially, only one third of people with RA test positive for the set of antibody called the rheumatoid factor (Rf). Most people with rheumatoid arthritis will eventually develop this marker and a positive Rf is considered a sign and symptom of rheumatoid arthritis. However, some people test positive for rheumatoid factor, yet never develop the disease. The level of your Rheumatoid factor in the blood does not predict flares nor your outcome.
When your doctor says you’re seronegative (or sero negative), he’s indicating that you did not have more Rf than the normal population. Anti-CCP: These anti-CCP antibodies bind to some self proteins that are found predominately in the synovial tissue. The citrullinated proteins include filaggrin and its circular form (cyclic citrullinated peptide: CCP). The presence of these antibodies often correlates with some joint destruction. Although this test is relatively recent, a high level of anti-CCP is considered a sign and symptom of rheumatoid arthritis.
Inflammation: Inflammation is your body’s response to damage. Your body sends in certain types of white blood cells to pick up debris, fight off infection, promote healing and, if needed, bring in more blood vessels. There is usually a higher state of inflammation in rheumatoid arthritis patients and it is a classic sign and symptom of rheumatoid arthritis. These 2 tests are used to measure it. Erythrocyte sedimentation rate: This test, often called the ESR, or the sed rate measures the quantity and how quickly the cells are pelleted by spinning in a centrifuge. Indirectly, it measures how many cells are bigger and thus activated. C-reactive protein. A higher than normal level of C-reactive protein (CRP) in the blood also indicates that your body has chronic inflammation, and is a common sign and symptom of rheumatoid arthritis. However, high CRP is also found in chronic heart disease patients. General Health:Fatigue and a general sense of not feeling well are very common in RA patients. Some RA patients get flu-like symptoms, fever, chills whereas others do not. Rheumatoid arthritis affects different people differently. Some progress rapidly, some have arthritis for 1-2 years and then they go into remission. Others have arthritis that continually challenges them to find new approaches to reduce the pain and joint damage. Flare: Your RA pain and swelling increases and it can expand to include other joints. Remission: Your RA symptoms decrease and may disappear.
Many people with rheumatoid arthritis may also develop anemia, [a decrease in the production of red blood cells]. Other effects that occur less often include neck pain and dry eyes and mouth. Very rarely, people may have inflammation of the blood vessels, the lining of the lungs, or the sac enclosing the heart. Effect of Weather: Many RA patients say that they can detect when a change in weather is occurring. There have been a few studies: Some did not observe a significant correlation, whereas others reported: Women were more sensitive to weather than men (62% v 37%). Pain was increased with changes in barometric pressure and lower temperature Prevalence:There are approx. 2.1 million people diagnosed with Rheumatoid arthritis in the U.S. It occurs in all races and ethnic groups. While many cases begin in middle age, more cases begin in older people. There are some young people and children with a disease related to RA. It is called juvenile rheumatoid arthritis or juvenile inflammatory arthritis and is discussed further below.
RA occurs 2-3 times more frequently in women than men. This suggests that the sex hormones may influence its onset. Juvenile Rheumatoid ArthritisJuvenile rheumatoid arthritis is also known as Still's disease. There are about 285,000 children who have symptoms of juvenile rheumatoid arthritis in the U.S.
Juvenile rheumatoid arthritis (JRA) often begins in children with a high fever and shaking chills along with pain and swelling in many joints. A pink skin rash may be present. The painful joints do not completely resolve and are considered a classic sign and symptom of rheumatoid arthritis.
What are your sign and symptom of rheumatoid arthritis trying to tell you?Pain is one of your body’s ways to communicate that all is not well and that you need to change something(s). Learning to read your body’s pains and desires and acting accordingly can really help your body to heal.
When you change your viewpoint so that each pain, sign and symptom of rheumatoid arthritis is another clue in your puzzle, you’ll begin to see certain patterns.
Just like your conscious mind learns how to catch a ball, your autonomic nervous system figures out how to respond to changes in the amount of water you drink, your food and environment. [The autonomic nervous system is the part of your brain that oversees your breathing, muscles, digestion, blood flow, and other bodily functions.]
Once the autonomic nervous system decides how to respond to a given food or other item, it makes that same decision over and over again—regardless whether it’s the most comfortable for you or not.
Understanding your body’s responses and how it relates to your sign and symptom of rheumatoid arthritis can help you gain some control.
“Studies have shown that [rheumatoid arthritis] patients who are well informed and participate actively in their own care have less pain,” wrote the National Institute of Health branch, National Institute of Arthritis, Musculoskeletal and Skin Diseases.
You may sometimes choose to act like an arthritis detective. When you find an idea like “chronic dehydration causes joint pain”, you check whether this clue may apply to your case. For example, you would check to see if you drink as much water as recommended. If not, then you can increase the amount of water you drink to the recommended amount for a few weeks, months or so and see if it improves your health. And remember, you know your own body better than anyone else does.
Here are some potential areas that have acted as triggers for my and others’ rheumatoid arthritis. For more information, click on the links. (1) Do you have heartburn sometimes? Incomplete digestion of various foods can also flare your rheumatoid arthritis. About half of 50+ year olds have low stomach acid which causes incomplete digestion of meats, and most cases of heartburn. (Dr. Jonathan Wright finds that approx. half of his RA patients don’t digest their food well and when corrected, their symptoms lessen and often practically disappear!).
(2) When you’re stiff and aching, it’s hard to get up and move. How to lower the effects of your desk job with these 6 quick, easy exercises that increase your energy. (3) Exposure to man-made chemicals from foods, home and environment are hard to avoid—but here are 20 tips (4) Dehydration can cause the cartilage in your joints to change from smooth slippery surfaces to wrinkled, sticky surfaces--(Are your joints and cartilage thirsty?),
Hopefully some of these ideas will help you figure out what triggers your rheumatoid arthritis and give you sufficient strategies to reduce the pain, strengthen your hope, persistence and your determination. The mission of this web site is to give you the information you need to actively participate in your own care so that you too can live life to its fullest. If you have any questions, suggestions, or topics you’d like me to research and discuss, please send it in on the convenient contact page. Thanks! Note: Although I’ve had the sign and symptom of rheumatoid arthritis for 38 years, I rarely experience any pain now due to RA.
I'm sharing other tips in the free e-zine: Please note: the information on this website is a sharing of information and knowledge from the research and experience of Dr. Molnar-Kimber and her community. It is not intended to replace your one on one relationship with a qualified health care professional. It also is not intended to be medical advice. However, it is often observed that patients who take a major interest in their disease and learn as much as they can about their disease and potential treatments often improve faster than those who don’t. Dr. Molnar-Kimber encourages you to make your own health care decisions based upon your own research and discussions with your qualified health care professional. 2006 © Katherine L. Molnar-Kimber, Ph.D. |
Healing Choices for RA newsletter answers questions, provides tips, and discusses recent research on arthritis and other autoimmune diseases.